Varicose Vein Surgery
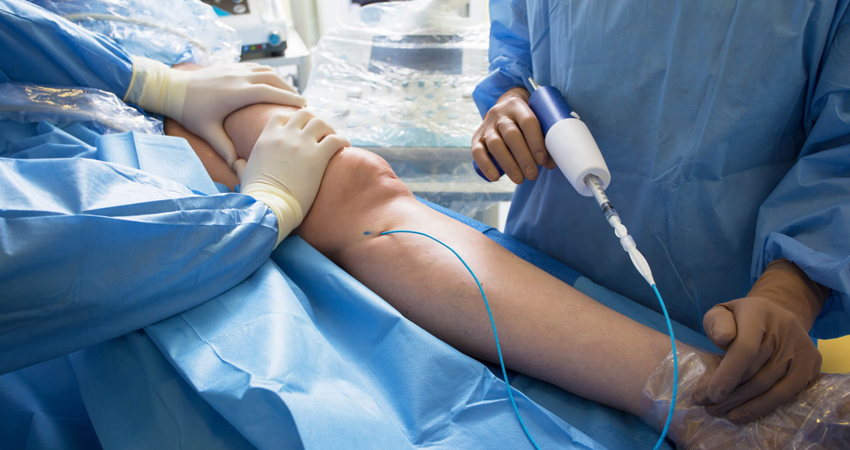
Varicose Vein Surgery
Varicose veins are a common vascular condition that could be both physically and emotionally challenging. Whether caused by genetics, lifestyle factors, or other underlying conditions, the presence of varicose veins can prompt individuals to seek effective solutions to alleviate the symptoms and enhance the overall quality of life. When it comes to addressing this disorder, varicose vein surgery emerges as a significant option for those affected. In this article, we provide a comprehensive guide on varicose vein surgery, providing insights about the procedure, empowering you to make informed decisions about your health and embark on a path toward improved well-being. Let’s begin with understanding the condition.
What are Varicose Veins?
Varicose veins are enlarged, twisted, and often swollen veins that typically appear blue or dark purple in color. They most commonly occur in the legs and can be seen through the skin. Varicose veins develop when the valves within the veins, which are responsible for regulating blood flow and preventing backward circulation, become weakened or damaged. As a result, blood pools in the veins, causing them to enlarge and become visibly prominent. Although lifestyle changes and conservative treatments can help manage symptoms, some individuals opt for varicose vein surgery for more significant relief and improved vascular health.
Who is Likely to Get Varicose Veins?
Although varicose veins can affect any individual, certain factors increase the likelihood of an individual developing this condition. These include:
- Genetics: Family history of varicose veins increases the risk, as inherited traits may include weakened vein walls or faulty valves.
- Age: Advancing age could be another contributing factor to varicose veins, as veins may lose elasticity and become more susceptible to damage over time.
- Gender: Women are more likely to develop varicose veins than men, with factors such as pregnancy, hormonal changes, puberty, and menopause influencing vein health.
- Weight and lifestyle: Being overweight or obese increases pressure on leg veins, and a lack of physical activity or a sedentary lifestyle can increase the risk of vein issues.
- Occupational factors: Jobs involving prolonged periods of standing or sitting may contribute to varicose veins, as a lack of movement can affect blood circulation and vein health.
- Hormonal influences: Hormonal fluctuations, such as those related to pregnancy or birth control use, can play a role in the development of varicose veins.
- Sun exposure: Excessive sun exposure may cause damage to the skin and veins, and sun-induced skin changes can affect the overall health of the veins.
- Other medical conditions: Conditions that increase abdominal pressure, such as constipation or tumors, can contribute, and a previous history of blood clotting may affect vein function.
Symptoms of Varicose Veins
Varicose veins can manifest with various symptoms, and individuals experiencing these signs may seek medical evaluation for further assessment. The symptoms of varicose veins include:
- Visible veins: Twisted, bulging veins that are visible beneath the skin, usually appearing dark blue or purple.
- Pain and discomfort: Aching or throbbing sensations in the legs, especially after prolonged standing or sitting.
- Swelling: The affected leg may exhibit swelling, particularly around the ankles and lower calf.
- Heaviness or fatigue: Individuals with varicose veins often report a sense of heaviness or fatigue in the legs.
- Itching and irritation: Some may experience itching or skin irritation around the affected veins.
- Cramps: Muscle cramps or a feeling of tightness in the leg muscles may occur.
- Skin changes: Over time, skin near the affected veins may undergo changes, such as discoloration, inflammation, or the development of sores or ulcers.
- Restlessness: Restless legs syndrome, characterized by an uncontrollable urge to move the legs, can be associated with varicose veins.
What is Varicose Vein Surgery?
Varicose vein surgery, also known as vein stripping or phlebectomy, is a medical procedure designed to treat and alleviate the symptoms of varicose veins. The surgery aims to remove or close off the damaged veins, redirecting blood flow to healthier veins, and is typically considered for individuals with symptomatic varicose veins that do not respond to conservative treatments or lifestyle changes. There are several surgical approaches, and the choice of method often depends on the severity of the varicose veins and the patient’s overall health.
What are the Types of Varicose Vein Surgery?
There are several types of varicose vein surgeries, each with its own approach to treating and managing varicose veins. Here are some common types of varicose vein surgeries:
- Vein stripping and ligation: A traditional surgical approach where the affected vein is physically removed through small incisions. Ligation involves tying off the vein to prevent blood flow before it is removed.
- Endovenous Laser Treatment (EVLT): A minimally invasive procedure where a thin laser fiber is inserted into the affected vein through a catheter. Laser energy is then delivered to heat and close off the vein, redirecting blood flow to healthier veins.
- Radiofrequency Ablation (RFA): Similar to EVLT, RFA uses radiofrequency energy instead of laser energy to heat and seal the diseased vein.
- Ambulatory phlebectomy: Involves the removal of smaller varicose veins near the surface of the skin through tiny incisions. Often performed on an outpatient basis.
- Endoscopic vein surgery: A less common procedure that involves the use of an endoscope to visualize and close off the affected vein through small incisions.
- Sclerotherapy: Sclerotherapy is not a surgical procedure, but a minimally invasive technique where a special solution is injected into the vein. The solution causes the vein to collapse and eventually be absorbed by the body.
- VenaSeal closure system: Involves the use of a medical adhesive to seal the affected vein, eliminating the need for heat-based methods.
- Microphlebectomy: A procedure in which small incisions are made to physically remove clusters of varicose veins near the surface of the skin.
- Glue embolization (Venaseal): Involves the use of a medical glue to seal the affected vein, similar to the VenaSeal Closure System.
What are the Benefits of Varicose Vein Surgery?
Varicose vein surgery can offer several benefits for individuals experiencing symptomatic varicose veins. While the specific advantages may vary depending on the type of surgery performed and individual health circumstances, the common benefits include:
Symptom relief: Varicose vein surgery is effective in relieving symptoms such as pain, aching, and discomfort associated with varicose veins. The surgery addresses the underlying cause, improving blood flow and reducing the pressure on the affected veins.
Improved circulation: By removing or closing off damaged veins, varicose vein surgery helps redirect blood flow to healthier veins. This can enhance overall circulation, reducing the risk of complications and promoting better vascular health.
Enhanced appearance: Surgery can improve the cosmetic appearance of the legs by eliminating or reducing the visibility of bulging, twisted varicose veins. This may lead to increased self-confidence and improved body image for individuals concerned about the appearance of their legs.
Prevention of complications: Varicose veins, if left untreated, may lead to complications such as venous ulcers, blood clots, or skin changes. Surgery can help prevent or mitigate these complications by addressing the underlying venous insufficiency.
Increased mobility: Reduced pain and discomfort can contribute to increased mobility and activity levels. Many individuals find that after surgery, they can engage in physical activities with greater ease and comfort.
What are the Complications or Side Effects of Varicose Vein Surgery?
Varicose vein surgery is generally considered safe, and serious complications are rare. However, as with any medical procedure, there are potential risks and side effects that individuals should be aware of. The specific complications can vary depending on the type of surgery performed and individual health factors. Common complications or side effects of varicose vein surgery may include:
- Pain or discomfort: Mild to moderate pain or discomfort is common after varicose vein surgery. This is usually temporary and can be managed with prescribed or over-the-counter pain medications.
- Bruising and swelling: Bruising and swelling around the incision sites are typical after surgery. These symptoms usually subside over time but may persist for a few weeks.
- Infection: Infections at the incision sites are rare but possible. It’s important to keep the surgical area clean and follow postoperative care instructions to minimize the risk of infection.
- Scarring: Surgical procedures involve incisions, and while efforts are made to minimize scarring, some degree of scarring is inevitable. The extent of scarring can vary based on the surgical technique and individual healing characteristics.
- Numbness or tingling: Some individuals may experience temporary numbness or tingling around the surgical area. This is typically a result of nerve irritation during the procedure and often resolves with time.
- Blood clots: Although rare, there is a small risk of blood clot formation (deep vein thrombosis) after varicose vein surgery. Patients are often encouraged to move and walk as soon as possible after the procedure to minimize this risk.
- Allergic reactions: In procedures involving the use of medical adhesives or sclerosing agents, there is a minimal risk of allergic reactions. This risk is generally low, and complications can be effectively managed by healthcare providers.
- Recurrence: While surgery is designed to treat varicose veins effectively, there is a possibility of vein recurrence over time. Regular follow-up with a healthcare provider is essential to monitor and address any potential issues.
-

Cashless Facility Available
-

All mediclaim/Health Insurance Accepted
-

EMI Payment Option Available
-

Free Guidance to choose right Health Insurance
-

Home Visit Available
